Human reproductive anatomy is a foundational topic in medical science, biology education, and health literacy. Whether you are studying anatomy diagrams, reviewing textbook material, or building educational resources, a clear understanding of male and female reproductive structures—and how they function—is essential.
This guide explores the anatomical components, physiological roles, and structural differences between the sexes, supported by references commonly found in medical textbooks such as Gray’s Anatomy, Moore’s Clinically Oriented Anatomy, and Guyton and Hall Textbook of Medical Physiology.
Quick Takeaways
- The reproductive system enables the production of gametes (sperm and ova), fertilization, and—biologically in females—pregnancy and childbirth.
- Male anatomy is primarily designed for sperm production and delivery.
- Female anatomy supports ovum production, fertilization, implantation, gestation, and birth.
- Hormones regulate reproductive structure and function in both sexes.
- Internal and external reproductive organs work together in coordinated systems.
- Structural differences reflect functional specialization rather than hierarchy.
Overview of the Human Reproductive System
The human reproductive system differs from most other organ systems because it is not essential for individual survival—but it is essential for species continuation.
It consists of:
- Primary sex organs (gonads): Testes in males, ovaries in females
- Accessory ducts and glands
- External genitalia
- Hormonal regulatory systems (hypothalamus and pituitary interaction)
Reproductive anatomy is best understood through both structural diagrams and physiological function. Anatomy explains where and what; physiology explains how and why.
Male Reproductive Anatomy
The male reproductive system is organized around continuous sperm production and delivery.
1. Testes (Primary Gonads)

Location: Within the scrotum
Primary Functions:
– Produce sperm (spermatogenesis)
– Secrete testosterone
Inside each testis are seminiferous tubules, tightly coiled structures where sperm are produced. Interstitial (Leydig) cells between tubules produce testosterone.
Human Explanation Layer:
Think of the testes as both a factory and hormone center. They continuously produce sperm and release testosterone to regulate male secondary sexual characteristics such as muscle mass and voice depth.
2. Epididymis
A long, coiled tube resting on the posterior surface of each testis.
Function:
– Sperm maturation
– Sperm storage
Sperm leaving the testes are immature and non-motile. In the epididymis, they gain the ability to swim and fertilize an ovum.
3. Vas Deferens
A muscular duct that transports sperm from the epididymis to the ejaculatory duct.
During ejaculation, smooth muscle contractions propel sperm forward.
4. Accessory Glands
These glands contribute fluid that forms semen.
Seminal Vesicles
- Produce fructose-rich fluid
- Contribute ~60% of semen volume
Prostate Gland
- Adds alkaline fluid
- Enhances sperm motility
Bulbourethral (Cowper’s) Glands
- Secrete lubricating pre-ejaculate
- Neutralize acidic urine residue
5. Penis
The external organ responsible for:
- Sexual intercourse
- Delivery of semen
- Urination (shared urethral pathway)
It contains erectile tissue (corpora cavernosa and corpus spongiosum) that fills with blood during arousal.
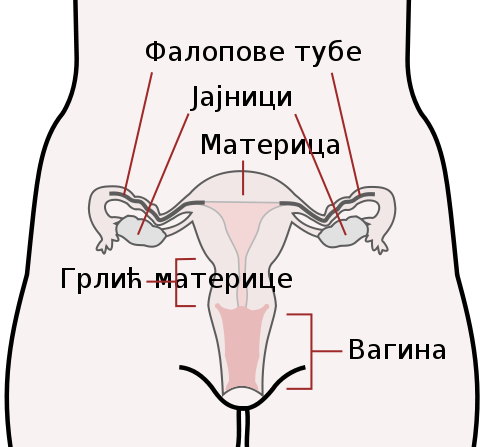
Female Reproductive Anatomy
The female reproductive system is cyclic and highly regulated, supporting fertilization, implantation, pregnancy, and childbirth.
1. Ovaries (Primary Gonads)
Location: Lateral pelvic cavity
Functions:
– Produce ova (oogenesis)
– Secrete estrogen and progesterone
Unlike continuous sperm production in males, females are born with a finite number of follicles.
Human Explanation Layer:
If the testes are factories, the ovaries are more like a vault and timing system—releasing one mature ovum approximately once per menstrual cycle.
2. Fallopian Tubes (Uterine Tubes)
Connect ovaries to the uterus.
Function:
– Capture ovulated egg
– Site of fertilization (usually in the ampulla)
Cilia lining the tube help move the egg toward the uterus.
3. Uterus
A muscular, pear-shaped organ divided into:
- Fundus
- Body
- Cervix
Function:
– Implantation of fertilized egg
– Support of fetal development
– Contraction during childbirth
The inner lining, called the endometrium, thickens during the menstrual cycle in preparation for implantation.
4. Cervix
The lower portion of the uterus opening into the vagina.
Functions:
– Produces cervical mucus
– Dilates during childbirth
– Acts as a protective barrier
5. Vagina
A muscular canal connecting the cervix to the external genitalia.
Functions:
– Receives penis during intercourse
– Birth canal
– Exit for menstrual flow
6. External Genitalia (Vulva)
Includes:
- Labia majora
- Labia minora
- Clitoris
- Vestibule
The clitoris contains erectile tissue and is highly innervated, playing a central role in sexual arousal.
Hormonal Regulation in Both Sexes
Reproductive anatomy does not function independently—it is regulated by the hypothalamic-pituitary-gonadal (HPG) axis.
Key Hormones:
- Gonadotropin-releasing hormone (GnRH)
- Luteinizing hormone (LH)
- Follicle-stimulating hormone (FSH)
- Testosterone (male)
- Estrogen and progesterone (female)
In males, hormone levels remain relatively stable after puberty.
In females, hormonal changes follow a cyclical pattern (menstrual cycle).
Major Structural Differences Between Male and Female Reproductive Systems
| Feature | Male Anatomy | Female Anatomy |
|---|---|---|
| Primary Gonads | Testes | Ovaries |
| Gamete Production | Continuous after puberty | Cyclical, finite reserve |
| Hormonal Pattern | Relatively stable | Cyclical |
| External Genitalia | Penis and scrotum | Vulva |
| Site of Fertilization | External to body | Internal (fallopian tube) |
| Gestation | Not applicable | Uterus supports pregnancy |
| Urethra Function | Urinary + reproductive | Urinary only |
Functional Comparison: Efficiency vs. Complexity
The male reproductive system prioritizes:
– Volume of gamete production
– Efficient delivery
The female reproductive system prioritizes:
– Selection and maturation of one ovum per cycle
– Protection and nourishment of developing embryo
– Hormonal synchronization
This reflects biological specialization rather than superiority.
Understanding Reproductive Anatomy Through Medical Diagrams
Medical anatomy diagrams typically show:
- Sagittal (side) view of pelvis
- Frontal view of internal structures
- Cross-sectional vascular supply
- Histological sections (microscopic anatomy)
Textbooks such as:
– Gray’s Anatomy: The Anatomical Basis of Clinical Practice
– Moore’s Clinically Oriented Anatomy
– Netter’s Atlas of Human Anatomy
– Guyton and Hall Textbook of Medical Physiology
provide high-quality, labeled illustrations used in medical training.
When reviewing diagrams, focus on:
– Relative positioning
– Vascular supply
– Nerve innervation
– Structural relationships
Understanding spatial arrangement is key to interpreting pathology and clinical procedures.
Clinical Relevance of Reproductive Anatomy
A clear anatomical understanding helps explain:
- Infertility causes
- Ectopic pregnancy
- Prostate enlargement
- Testicular torsion
- Endometriosis
- Polycystic ovary syndrome (PCOS)
- Erectile dysfunction
For example:
– A blockage in the vas deferens prevents sperm transport.
– Damage to fallopian tubes increases ectopic pregnancy risk.
– Prostate enlargement can compress the urethra.
Anatomy directly informs diagnosis and treatment.
Developmental Differences and Embryology (Brief Overview)
Male and female reproductive systems originate from similar embryological structures.
- Wolffian ducts → male internal structures
- Müllerian ducts → female internal structures
Sex differentiation begins around week 7 of embryonic development.
This shared origin explains some anatomical similarities.
Frequently Asked Questions (FAQs)
1. Why are the testes located outside the body?
Sperm production requires a temperature slightly lower than core body temperature. The scrotum regulates this temperature.
2. Do females produce eggs continuously like males produce sperm?
No. Females are born with all their primary oocytes. One typically matures per cycle until menopause.
3. Where does fertilization usually occur?
In the ampulla of the fallopian tube.
4. Can reproductive anatomy vary?
Yes. Natural anatomical variations occur. Intersex variations also exist and reflect differences in sex development.
5. Is the urethra part of the reproductive system in both sexes?
In males, yes (shared urinary and reproductive pathway).
In females, the urethra is only part of the urinary system.
Common Misconceptions
Misconception: The vagina and vulva are the same.
Correction: The vulva is external; the vagina is the internal canal.
Misconception: The prostate produces sperm.
Correction: Sperm are produced in the testes. The prostate contributes fluid.
Misconception: Fertilization happens in the uterus.
Correction: It usually occurs in the fallopian tube.
Practical Learning Tips for Students
- Label blank diagrams repeatedly.
- Use 3D anatomical models or digital simulations.
- Trace the path of gametes (sperm and egg).
- Link structures to functions.
- Study histology alongside gross anatomy.
Understanding improves when structure is tied to purpose.
Conclusion
Human reproductive anatomy reflects biological specialization for gamete production, fertilization, and—within female anatomy—gestation and childbirth.
The male system emphasizes continuous production and efficient delivery of sperm.
The female system emphasizes cyclical regulation, ovum release, fertilization, implantation, and fetal support.
This knowledge forms the foundation for advanced study in medicine, nursing, physiology, obstetrics, gynecology, urology, and reproductive health sciences.