Understanding Human Reproductive Anatomy: A Comprehensive Guide to Male and Female Systems
Human reproductive anatomy is a cornerstone of medical education, clinical practice, and health literacy. Whether studying medical anatomy diagrams, preparing for healthcare exams, or seeking a deeper understanding of how the body functions, knowledge of the male and female reproductive systems is essential.
This guide provides a detailed yet reader-friendly explanation of reproductive organs, their functions, anatomical differences between sexes, and how they work together in reproduction. It integrates textbook-based anatomical detail with clear human explanations and practical examples to support real-world understanding.
Quick Takeaways
- The male reproductive system is primarily responsible for producing, storing, and delivering sperm.
- The female reproductive system produces eggs (ova), supports fertilization, and sustains pregnancy.
- Both systems include external and internal structures that work together in coordinated hormonal cycles.
- Hormones such as testosterone, estrogen, progesterone, FSH, and LH regulate reproductive development and function.
- Structural differences reflect distinct biological roles in reproduction.
- Reliable anatomy references include Gray’s Anatomy, Moore’s Clinically Oriented Anatomy, and Netter’s Atlas of Human Anatomy.
Why Understanding Reproductive Anatomy Matters
Reproductive anatomy is not only relevant for reproduction itself. It plays a crucial role in:
- Puberty and sexual development
- Hormonal regulation
- Fertility and infertility treatment
- Cancer screening (e.g., prostate, cervical, ovarian)
- Urological and gynecological health
- Sexual health education
Understanding structure helps explain function. For example, knowing where the ovaries are located clarifies why ovarian pain may be felt in the lower abdomen. Recognizing the prostate’s position helps explain urinary symptoms when it enlarges.
Overview of the Male Reproductive System

The male reproductive system consists of external and internal structures designed to produce and transport sperm.
External Male Reproductive Structures
1. Penis
Function: Delivers sperm into the female reproductive tract during intercourse; also allows urination.
The penis contains three columns of erectile tissue:
– Two corpora cavernosa
– One corpus spongiosum (surrounding the urethra)
During sexual arousal, blood fills these tissues, causing erection. This vascular mechanism is essential for successful sperm delivery.
Human explanation: Think of the erectile tissue as sponge-like cylinders that fill with blood when stimulated, similar to inflating a soft structure from within.
2. Scrotum
Function: Protects and regulates temperature of the testes.
The scrotum is a skin-covered sac containing:
– Testes
– Epididymides
– Part of the spermatic cord
Sperm production requires a temperature slightly lower than core body temperature (about 2–3C lower). Muscles in the scrotum adjust its position to maintain optimal temperature.
3. Testes
Function: Produce sperm (spermatogenesis) and testosterone.
Inside each testis are:
– Seminiferous tubules (site of sperm production)
– Leydig cells (produce testosterone)
Spermatogenesis is a continuous process beginning at puberty and lasting throughout life, although it declines with age.
Internal Male Reproductive Structures
1. Epididymis
A tightly coiled tube on the posterior surface of each testis.
Function: Sperm maturation and storage.
Newly produced sperm are immature and non-motile. In the epididymis, they gain motility and fertilizing ability.
2. Vas Deferens
A muscular tube that transports sperm from the epididymis to the ejaculatory ducts.
During ejaculation, muscular contractions propel sperm forward.
3. Seminal Vesicles
Paired glands that secrete fluid rich in:
– Fructose (energy source for sperm)
– Prostaglandins
– Clotting proteins
This fluid forms a large portion of semen.
4. Prostate Gland
Located below the bladder, surrounding part of the urethra.
Function: Adds alkaline fluid to semen to neutralize vaginal acidity.
Clinical note: Prostate enlargement (BPH) can compress the urethra and affect urination.
5. Bulbourethral (Cowper’s) Glands
Produce a lubricating pre-ejaculatory fluid that neutralizes urethral acidity.
Overview of the Female Reproductive System
The female reproductive system is structurally more complex because it must support fertilization, implantation, and pregnancy.
External Female Reproductive Structures (Vulva)
The vulva includes:
- Labia majora
- Labia minora
- Clitoris
- Vestibule
- Vaginal opening
Clitoris
A highly innervated erectile structure homologous to the male penis. It contains erectile tissue and plays a central role in sexual arousal.
Internal Female Reproductive Structures
1. Ovaries
Function: Produce ova (eggs) and hormones (estrogen, progesterone).
Each month (on average), one ovary releases an ovum during ovulation. The ovaries also regulate menstrual cycles via hormone production.
Human explanation: The ovaries act like a hormonal control center and an egg reservoir combined.
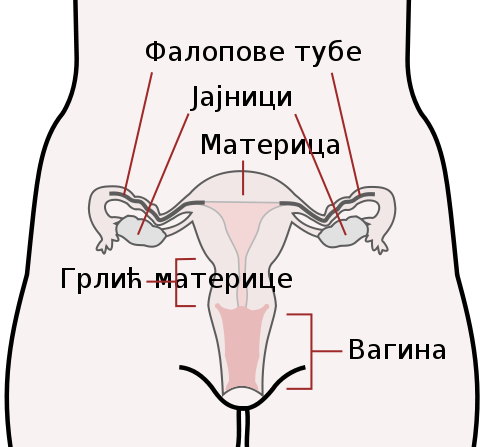
2. Uterine (Fallopian) Tubes
Connect ovaries to the uterus.
Function: Site of fertilization.
Finger-like projections (fimbriae) sweep the ovulated egg into the tube. Cilia help move it toward the uterus.
3. Uterus
A muscular organ with three layers:
– Endometrium (inner lining)
– Myometrium (muscular layer)
– Perimetrium (outer layer)
Function: Supports implantation and fetal development.
If fertilization does not occur, the endometrial lining sheds during menstruation.
4. Cervix
Lower portion of the uterus opening into the vagina.
Function: Produces cervical mucus and acts as a barrier or gateway depending on cycle phase.
Cervical screening (Pap smear) detects precancerous changes.
5. Vagina
A muscular canal connecting the cervix to the external body.
Functions:
– Receives penis during intercourse
– Birth canal
– Outlet for menstrual flow
Hormonal Regulation in Both Sexes
Reproductive anatomy does not function independently of the endocrine system.
Key Hormones
| Hormone | Produced By | Primary Function |
|———-|————-|—————–|
| Testosterone | Testes | Male secondary sexual characteristics, sperm production |
| Estrogen | Ovaries | Female secondary sexual characteristics, endometrial growth |
| Progesterone | Ovaries | Maintains uterine lining |
| FSH | Pituitary gland | Stimulates gamete production |
| LH | Pituitary gland | Triggers ovulation; stimulates testosterone production |
The hypothalamic–pituitary–gonadal (HPG) axis regulates reproductive function in both sexes.
Key Differences Between Male and Female Reproductive Anatomy
The anatomical differences reflect distinct biological roles.
| Feature | Male | Female |
|———-|——|——–|
| Primary gamete | Sperm | Ovum |
| Gamete production | Continuous | Cyclical |
| External genitalia | Prominent | Less prominent |
| Hormonal cycle | Relatively stable | Monthly cyclic changes |
| Role in reproduction | Delivers sperm | Supports fertilization, gestation, birth |
Structural Homologies Between Sexes
Some structures share embryological origins:
| Male Structure | Female Equivalent |
|—————|——————|
| Penis | Clitoris |
| Scrotum | Labia majora |
| Testes | Ovaries |
Understanding these homologies clarifies why tissues share similarities in nerve supply and erectile capability.
Clinical Correlations
Male Conditions
- Benign Prostatic Hyperplasia (BPH)
- Prostate cancer
- Testicular torsion
- Varicocele
- Erectile dysfunction
Female Conditions
- Polycystic Ovary Syndrome (PCOS)
- Endometriosis
- Uterine fibroids
- Cervical cancer
- Ovarian cysts
Understanding anatomy improves diagnostic reasoning. For example, pelvic inflammatory disease often spreads along the uterine tubes because they provide a direct anatomical pathway.
Medical Anatomy Diagrams: How to Read Them Effectively
Medical diagrams often show:
- Sagittal (side) views
- Coronal (front) views
- Cross-sections
- Labeled vascular and nerve supply
When studying diagrams:
- Identify orientation (anterior vs posterior).
- Recognize scale—organs may be enlarged for clarity.
- Note relationships between organs (e.g., bladder anterior to uterus).
- Cross-reference with atlas images.
Recommended references:
- Gray’s Anatomy: The Anatomical Basis of Clinical Practice
- Moore, Dalley & Agur – Clinically Oriented Anatomy
- Netter’s Atlas of Human Anatomy
- Snell’s Clinical Anatomy
These textbooks provide reliable, peer-reviewed anatomical illustrations widely used in medical education.
Reproductive Anatomy Across the Lifespan
Before Puberty
Reproductive organs are immature and hormonally inactive.
Puberty
Hormonal activation leads to:
– Growth of reproductive organs
– Development of secondary sexual characteristics
– Onset of sperm production and menstruation
Adulthood
Peak reproductive capacity occurs in early adulthood.
Aging
- Male: Gradual testosterone decline.
- Female: Menopause marks cessation of ovarian function.
A Human Explanation Layer: How It All Works Together
Imagine reproduction as a coordinated biological relay:
- The male system produces and prepares sperm.
- The female system prepares a nutrient-rich environment monthly.
- Fertilization occurs in the uterine tube.
- The uterus transforms into a life-support system.
Each organ plays a specialized yet interconnected role. Remove or impair one component, and the entire system adapts or struggles.
Frequently Asked Questions (FAQs)
1. Why are the testes located outside the body?
Sperm production requires a slightly cooler temperature than core body temperature. The scrotum regulates this temperature.
2. What is the most common site of fertilization?
The ampulla of the uterine (fallopian) tube.
3. Can reproductive anatomy vary between individuals?
Yes. Variations such as uterine shape differences or undescended testes occur and may or may not affect fertility.
4. Why does the menstrual cycle occur monthly?
It reflects cyclical hormonal changes that prepare the uterus for potential pregnancy.
5. Are male and female reproductive organs completely different?
No. Many structures share embryological origins, explaining structural similarities.
Conclusion
Understanding human reproductive anatomy requires more than memorizing organ names. It involves recognizing:
- Structural relationships
- Functional coordination
- Hormonal regulation
- Clinical relevance
- Sex-based differences
The male system focuses on continuous gamete production and delivery, while the female system operates cyclically and supports fertilization, implantation, and pregnancy.
Using reliable anatomical textbooks and well-labeled diagrams enhances both academic study and practical healthcare understanding. Whether for medical education, patient awareness, or professional training, a solid grasp of reproductive anatomy forms a critical foundation in human biology.